Endocrinologists are used to people not knowing what they do. Patients often assume that, for example, Dr. Rasa Kazlauskaite spends her days focused on the “love hormones,” like testosterone and estrogen. She reminds them that we all have a variety of hormones and hormone-producing glands with important jobs—including the pituitary gland, which oversees everything from growth to metabolism, and adrenal glands, which produce the stress hormone cortisol.
Plus, endocrinologists treat conditions like diabetes, thyroid disease, polycystic ovary syndrome, and even osteoporosis. “We also help people figure out the causes of increased weight and help them lose weight and improve their metabolism,” says Kazlauskaite, who’s the director of the diabetes technology program at Rush University Medical Center. In other words: Endocrinologists encounter a wide variety of symptoms all day, every day. Here are some surprising ones that concern them the most, even though patients don’t usually recognize that they might signal a problem.
A racing heart
When people notice their heart is racing, they often make an appointment with a cardiologist. But sometimes, they need an endocrinologist to get to the root cause—because it’s one of the most common symptoms of hyperthyroidism, says Dr. Rachel Pessah-Pollack, a clinical associate professor in the division of endocrinology, diabetes, and metabolism at NYU School of Medicine. “They’ll say they were having palpitations, they were feeling winded, and they looked at their Apple Watch, and their heart rate was up,” she says. (Anything over 100 beats per minute, for a few days in a row, is generally considered elevated.)
Read More: 9 Weird Symptoms Cardiologists Say You Should Never Ignore
Fortunately, if it turns out to be an overactive thyroid, there are a variety of treatment options, Pessah-Pollack reassures her patients. Depending on what’s causing it—Graves disease or noncancerous growths, for example—that might mean medication or surgery to remove all or part of the thyroid gland. Sometimes, very little treatment is needed: In recent years, endocrinologists have reported a COVID-19-related increase in thyroiditis, or inflammation that can cause hyperthyroidism. “The key with that diagnosis is that it actually often resolves on its own,” Pessah-Pollack says. “No treatment needed, other than a heart-rate medication.”
Itchiness and redness in the groin area, along with increased thirst
Young people, in particular, often show up at the hospital or in their primary care doctor’s office complaining about a rash in their groin area. They assume they have a sexually transmitted infection, Kazlauskaite says—but as it turns out, the rash was preceded or accompanied by increased thirst and hunger, and they actually have a yeast infection caused by newly developed diabetes. “It’s an unfortunate symptom,” she acknowledges. “But people need to know so they can get treated.” Yeast feeds off sugar, Kazlauskaite explains, which is why infections are often triggered by out-of-control blood sugar levels. In addition to figuring out the best way to treat a patient’s diabetes, doctors will typically treat the yeast infection with an antibiotic or over-the-counter antifungal cream.
New anxiety
An overactive thyroid can cause “significant mood changes” and severe anxiety, Pessah-Pollack says. She regularly sees patients who describe being nervous all the time—and she sometimes even notices that their hands are shaking. “If you’re somebody who’s always kind of been calm, and then all of a sudden you’re continuously anxious, it can be a trigger to evaluate for hyperthyroidism,” she says. That’s especially true if you’re also experiencing other symptoms of an out-of-whack thyroid, like unexplained weight changes, trouble sleeping, or frequent diarrhea. Instead of brushing it off and assuming work or money must be getting to you, bring it up with your doctor. There’s no harm in exploring whether your thyroid could be to blame.
A hump between your shoulders
Having too much cortisol can cause Cushing syndrome, which is most common in women and affects about 10 to 15 million people per year. The condition leads to rapid weight gain—but the extra pounds don’t always show up in the stomach. Instead, some people gain weight in their face (which is called “moon face”) or develop a “buffalo hump” on their neck, in between their shoulders. “It occurs when the body is putting out too much cortisol for a long time,” Pessah-Pollack says. “Normally, cortisol helps our body function. But if you have too much, you get classic findings on the body.” In addition to a hump between the shoulders, you might also notice you have dark pink or purple stretch marks on your stomach, thighs, or breasts, and that while your upper body is larger, your arms and legs are quite thin.
Read More: Should You Use Retinol and Retinoids?
If Pessah-Pollack suspects high cortisol levels, she orders a saliva-based test or timed urine collection, which requires peeing in a special container over a 24-hour period. Then, she has to figure out the underlying cause: Is it a tumor in the pituitary gland or the adrenal glands? Is the patient taking synthetic hormone medicines that might be to blame? Depending on what’s driving someone’s Cushing syndrome, treatment could be surgery or hormone-inhibiting medication.
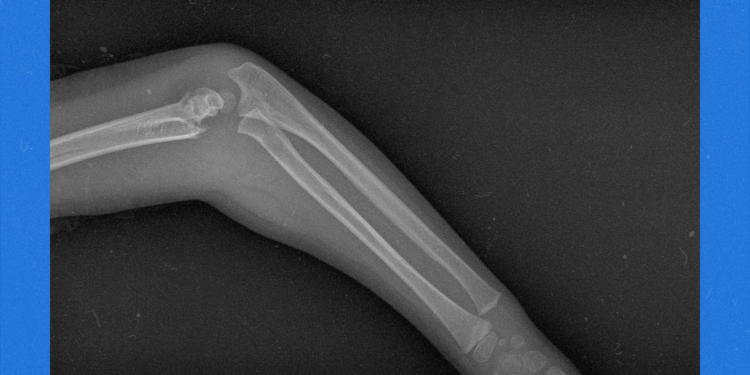
Sudden fractures
You might not think of brittle bones as part of endocrinologists’ domain—but these doctors, in addition to rheumatologists, diagnose and treat osteoporosis. Kazlauskaite pays special attention to fragility fractures, which are fractures caused by only minor trauma, or without any cause at all. (Think: Breaking a rib after coughing, sneezing, or getting a hug, or fracturing your tailbone after sitting on a bench.)
Metabolic bone disease has a variety of underlying causes. Some people, for example, don’t get enough of important minerals, like calcium, magnesium, or vitamin D. Kazlauskaite recalls a 42-year-old patient who showed up to her first appointment in a wheelchair, unable to lift her weak arms or legs. “We diagnosed her with severe vitamin D deficiency,” she says. “It took me six months to build her bones, and then she prances into my office and says, ‘Look, doctor, I don’t even use a cane.’” Other times, it might turn out that diabetes is causing brittle bones, increasing the risk of a fracture. Kazlauskaite spends time figuring out the underlying cause, and then typically recommends patients take certain supplements and medication, while making dietary changes and implementing more weight-bearing exercises.
Feeling too hot or cold
Abrupt changes in a person’s temperature can signal that something is going on with their thyroid. Pessah-Pollack’s patients, for instance, often complain about sweating profusely and feeling hot all the time—yet they used to be the kind of people who never left home without a sweater. “It’s another sign that people sometimes ignore,” she says. “They just think, ‘Oh, I guess I’m changing. I’m just warm now.’” In reality, it could indicate hyperthyroidism, especially when paired with other symptoms.
Read More: Why Vinegar Is So Good for You
Meanwhile, some people might notice they can no longer tolerate the cold—which is one sign of hypothyroidism, or an underactive thyroid. The condition slows metabolism and triggers a drop in body temperature, which is why those who have it often report that they’re freezing, even in warm rooms.
Thinning eyebrows
Another classic sign of hypothyroidism is losing the outer third of your eyebrows, which is sometimes called “Queen Anne’s sign” in reference to an ancient portrait. “I had a patient who had thin eyebrows, and one side was just gone,” recalls Dr. Libu Varughese, an endocrinologist with Memorial Hermann Health System in Houston. Fortunately, thyroid-related hair loss is typically temporary, and with treatment, most people see their hair return to its baseline. Though truncated eyebrows might be aesthetically annoying, the diagnosis is nothing to stress about, he adds: “We have so many people on thyroid hormone replacement therapy.”
Having a narrower field of vision
If you’re suddenly struggling with your peripheral vision—which means you might feel like you’re looking into a tunnel, only able to see what’s straight in front of you—tell your doctor. You could have a pituitary tumor, which is a typically benign tumor in the brain.
Kazlauskaite, who works as an endocrinology consultant at a trauma center, often sees patients who were transported there after getting into a car accident. They undergo whole-body CT scans, and sometimes, pituitary tumors are discovered by chance. When that happens, the tumors are usually big enough to compress the optic nerve, which triggers vision loss. “Imagine you’re driving and changing lanes,” she says. “What happens? An accident, because you didn’t see that car.” This is an especially common way for men to learn they have a pituitary tumor, Kazlauskaite adds, since women will often first notice menstrual-cycle changes that encourage them to see a doctor. “In men, it’s more challenging because all the symptoms are gradual,” she says. “Even younger men say, ‘Oh yeah, I’m just getting older’”—when in reality, something more serious is going on.
Dangerously high blood pressure
If you have hypertension, you might blame genetics or your donut habit. Most people don’t realize it could be an endocrine problem, says Dr. Susan Samson, president of the American Association of Clinical Endocrinology. However, “There are endocrine causes of high blood pressure, and sometimes, they are not subtle.” Yet patients often misattribute them. At the most extreme level, for example, are tumors of the adrenal glands, or pheochromocytomas, which commonly lead to high blood pressure that reaches life-threatening levels. “Patients can have these incredibly high dangerous spikes in blood pressure and tremors and sweats, and they think, ‘Hey, that’s my heart,’” Samson says—but it’s not.
Read More: Is Adrenal Fatigue Real?
Other endocrine-related causes of high blood pressure could be at play, too, including high cortisol and excess levels of aldosterone, a hormone produced by the adrenal glands. If you’re on more than one hypertension medication, and your levels still haven’t improved, consider seeing an endocrinologist. “Maybe we can actually treat it and cure it instead of them having to be on multiple medications,” Samson says. “We’re always trying to educate our colleagues who are referring physicians about these things, but sometimes, they can be missed, and it takes time for someone else to recognize them.”
Poor exercise performance
Millions of men have low testosterone—and many more think they do, Samson says. For those who do, in fact, have too little of the male sex hormone, the signs can be subtle and nonspecific. Among them: loss of muscle mass and decreased fitness performance. “Men might be fatigued, or notice they’re working out at the gym like they used to, but their muscles are too tired or they’re too sore,” she says. “They’re not seeing any improvement. We call that exercise intolerance.” Low testosterone can affect many aspects of health, Samson adds—leading to a low sex drive, poor sleep, and mood changes—and is typically successfully treated with testosterone replacement therapy.
Breast discharge without having a baby
Sometimes, people who aren’t pregnant or postpartum start discharging breast milk—and while it’s most common among women, it can happen to men, too. “Women get scared, like, ‘Oh my God, I might have breast cancer,’” Kazlauskaite says. While it’s important to rule cancer out, this unusual symptom could also point to a prolactin-secreting benign tumor that lives in the pituitary gland—especially if paired with irregular menstrual periods. “Definitely see an endocrinologist,” she urges. There’s a range of treatments that can help reduce the prolactin and stop the milky discharge, including medication and surgery, and patients typically make a full recovery.
Enlarged hands and feet and widening gaps between the teeth
One of the conditions Samson treats is acromegaly, a rare hormonal disorder that occurs when the pituitary gland produces too much growth hormone. It causes bones and tissues to gradually grow in unusual ways: “These patients can actually have growth of their hands and feet, and changes in their facial features,” she says. People with the condition might notice their shoe size has gotten larger, for example, or that their rings no longer fit on their fingers.
Dental issues are also common. That could mean bite changes, tooth separation, an enlarged tongue, or a jaw that grows disproportionately. In fact, dentists are sometimes the first people to raise the alarm about acromegaly and refer their patients to endocrinologists. If it turns out someone does have the condition, they’ll often undergo surgery to remove their tumor; there are also therapies designed to lower growth hormone levels back to the normal range. “Some of the things don’t reverse—if bones have grown, they’re going to continue to have those changes,” Samson says. “But we do see improvement in some of the features because of the decrease in growth hormone. We know that if we normalize their growth hormone, then we normalize their mortality, and that’s really important to us as endocrinologists.”